Limb length discrepancy
Differences in leg length can arise from many and varied aetiologies.
Evidence Essentials has previously addressed aspects of this topic:
- 2017: https://angelaevanspodiatrists.com.au/evidence-essentials-blog-6-june-2017/
- 2020: https://angelaevanspodiatrists.com.au/galeazzis-test-a-useful-assessment-method-for-paediatric-limb-length-inequality/
Limb length discrepancy (LLD) may be of greater or lesser clinical significance, symptomatic or not, more or less innocuous.
An average LLD of 1.6 ± 2.3 cm (2.2% ± 4.5%) difference in leg length, probably has little real difference in gait between the short and long sides. It has also been shown, that LLD of 6.5 ± 2.8 cm, or a difference more than 5.5% between the legs, patients toe-walked on the short side
[Song KM, Halliday SE, Little DG: The effect of limb-length discrepancy on gait. J Bone Joint Surg Am 1997;79:1690-1698.]Whilst many studies report correlation between LLD and back pain, and also scoliosis, causation has not been established [Hubbard EW et al, J Am Acad Orthop Surg 2019;27:312-319 DOI: 10.5435/JAAOS-D-18-00143].
Coincidentally, in the last two days, I have seen four paediatric cases with varied presentations of LLD:
Case 1: age 20 years, male
History of R femoral tumour at age 11 years (presented as night time leg pain). Excision resulted in LLD of 4 to 5cm. Following chemotherapy for the cancer, R shoe build-ups have been used throughout growth. He is now awaiting an orthopaedic lengthening procedure, including external Ilizarov ring fixation. He had had low back pain prior to the R shoe build ups.
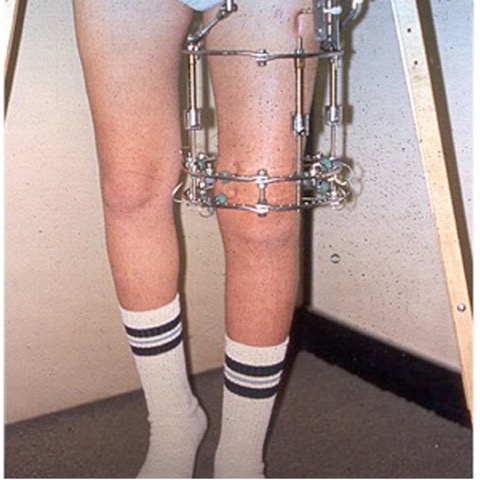
Figure 1: Ilizarov apparatus, traction between rings adjusted for gradual bone growth.
Case 2: age 4 years, female
Developmental hip dysplasia, which unfortunately (and unusuallY0 was not detected until aged over 2 years. She is a third child, was not breech presentation, and birth weight 3.2 kgs. She had a mild limp, but this had been regarded as ‘muscular’. Once diagnosed, she underwent pre-operative traction, ORIF and spica cast, followed by Pavlik harness full-time for 3 months (until aged almost 3 years). She walked again independently at 3.5 years.
The surgeon referred her to me concerned about her L abducted angle of gait, and flatter L foot. This has been stabilised with adapted generic foot orthoses, resulting in L=R gait angles, and even PSIS in stance.

Figure 2: Radiographic view of hips, recovering L DDH at age 4 years.
Case 3: age 17 years, male
History of L femoral fracture at age 4 years. Underwent ORIF. Has had LLD approximating 2 to 3.5 cm between ages 5 to 15 years. In-shoe raises have been used periodically across growth. Clinically, LLD has now reduced to < 1cm, and no extrinsic adjustment is used. He is symptom free, and almost 190cm height.
Case 4: age 27, female
No history of either lesion nor injury, but an evident LLD from age 3 to 4 years. Back pain intermittently since teen age, but also a successful sporting history playing hockey, and very good general health. The LLD origin is shortness of L femur, presenting as Galeazzi’s sign, with no Trendelenburg sign. The shorter L leg is smaller in circumference (full length) and is non-dominant and hence, less ‘used’. LLD approximates 3 cm, and this patient is happy with her 1.5 cm L shoe build up, with in-shoe modifications providing another 1cm raise. She is asymptomatic, unless barefoot for longer periods (eg 2 to 3 days, provokes low back pain).
These cases represent only four aetiologies for LLD presentation: tumour
DDH
fracture
congenital.
There are many other aetiologies, including: hemihypertrophy
hypoplasia
hemimelia
hemiplegia
[Evans AM, Paediatric Podiatry, Chapter 12; IN: Neale’s Disorders of the Foot and Ankle 9th EditionEds: Burrow, Rome, Padhiar; Elsevier, 2020; pages 298-338].
It is worth thinking about LLD from the perspective children’s legs growth. Early in development, leg length approximates 35% of height. By skeletal maturity, the legs account for almost 50% of height; and so, leg length accounts for a greater proportion of height as children grow older
[Iobst C: Growth of the musculoskeletal system, in Martus J, ed: Orthopaedic Knowledge Update Pediatrics, ed 5. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2016, pp 59-68.]
Figure 3: Radiograph showing the percentage contribution of the femoral and tibial physes to bone growth, lower limb growth, and average annual growth of each physis.
[Hubbard EW et al, J Am Acad Orthop Surg 2019;27:312-319 DOI: 10.5435/JAAOS-D-18-00143].The general recommendation for management of LLD is that LLD predicted to be less than 2 cm at skeletal maturity do not require surgical intervention; and LLD of 2 to 4 cm at maturity may have contralateral epiphysiodesis in the skeletally immature patient
[Vitale MA, Choe JC, Sesko AM, et al: The effect of limb length discrepancy on health relatedquality of life: Is the “2 cm rule” appropriate? J Pediatr Orthop B 2006;15: 1-5].
Many studies have shown that healthy asymptomatic people can have up to a 2 cm LLD found incidentally. Hence, the common premise that discrepancies less than 2 cm at skeletal maturity can be left alone, observed, or use an in-shoe raise. Clearly, an unacceptable angular deformity in the short limb, or symptomatic LLD will requires (some form of) treatment
[Hubbard EW et al, J Am Acad Orthop Surg 2019;27:312-319 DOI: 10.5435/JAAOS-D-18-00143].Please join the Green Podiatry campaign: https://angelaevanspodiatrists.com.au/green-podiatry/
Evidence Essentials is non-profit, proceeds directed to APERF (Australasian Podiatric Education and Research Foundation) https://www.podiatry.org.au/about/aperf/aperf505
Please keep an eye out for the Evidence Essentials blogs and enjoy the FREE resources https://angelaevanspodiatrists.com.au/category/resources/
Thank you for reading this Evidence Essentials blog post.
Kind regards,
Angela Evans
Dr Angela Evans AM
PhD, FFPM RCPS(Glasg)
